 Door County Medical Center's surgical suites recently underwent a procedure of their own! Over the past couple of months, the surgical suites have been upgraded with new, state-of-the-art equipment and additional integration. To learn more about the new and improved surgical suites we spoke with Gwen Haight, MSN, RN—about what equipment has been upgraded, how the upgrade is progressing, and what it means for both DCMC's surgical teams and for patients.
Door County Medical Center's surgical suites recently underwent a procedure of their own! Over the past couple of months, the surgical suites have been upgraded with new, state-of-the-art equipment and additional integration. To learn more about the new and improved surgical suites we spoke with Gwen Haight, MSN, RN—about what equipment has been upgraded, how the upgrade is progressing, and what it means for both DCMC's surgical teams and for patients.
As Director of Perioperative Services, Haight oversees the surgical department, including preoperative (patient admissions and preparation), intraoperative (the surgical team that works in the operating room), the post anesthesia care unit (the recovery room, or time immediately following surgery/anesthesia) and postoperative (the period getting patients mobile and discharged). Note: portions of the interview have been edited for length and clarity.
•
How has the upgrade to the surgical suites been progressing and where are we in the process? In other words, what has been upgraded so far?
It's important to note that the equipment we had was high quality and worked well, but it is about eight years old, and technology has had many advances in eight years. Our primary concern was the equipment was becoming outdated.
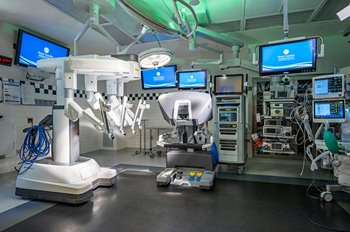
 The operating rooms are still laid out in the same fashion as they were prior to the upgrades. Primarily, the upgrades are to the equipment. There have been two phases to the project. The first phase has been completed and focused on the majority of the fixed equipment in the operating room, consisting of new surgical booms, operating room light, screens and a central control monitor or hub.
The operating rooms are still laid out in the same fashion as they were prior to the upgrades. Primarily, the upgrades are to the equipment. There have been two phases to the project. The first phase has been completed and focused on the majority of the fixed equipment in the operating room, consisting of new surgical booms, operating room light, screens and a central control monitor or hub.
Surgical booms hang from the ceiling and provide shelves for holding equipment, provide gas and electrical outlets, and hold the different cables and cords, keeping them off of the floor. The booms rotate and swing into different positions and locations to accommodate a particular type of surgery and/or the needs of the surgical team. The new booms are lightweight, streamlined, employ button control to move up and down, and lock into place. Perhaps most importantly, they move with ease—our prior booms were heavy, hard to move, and had become cumbersome and restrictive with regard to changing the setup of the room.
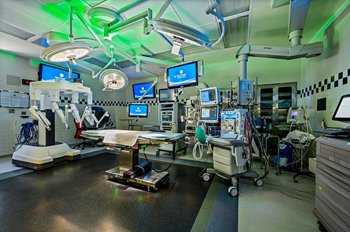
 With the screens, the change comes down to number and size. Where we previously relied on two 24-inch screens, now each surgical suite has five high-definition display screens ranging between 40 to 50 inches in size—more than doubling the number and size of our previous screens, as well as the capacity of what can be viewed at any given time during the procedure.
With the screens, the change comes down to number and size. Where we previously relied on two 24-inch screens, now each surgical suite has five high-definition display screens ranging between 40 to 50 inches in size—more than doubling the number and size of our previous screens, as well as the capacity of what can be viewed at any given time during the procedure.
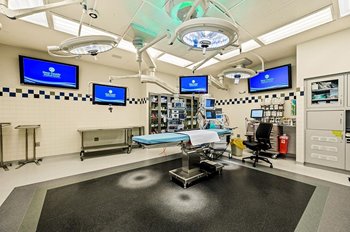
We now have a central control monitor or hub. This allows us to manage various equipment that is housed on the booms—all from this central location and at the fingertips of the nurse. This improves efficiency by giving us seamless connectivity to images, data, and settings for the equipment, all in one location.
Additionally, we now have overhead music in the surgical suite, so patients can choose what they would like to listen to as they fall asleep. We also have the capability to show movies or have different scenes or sounds on the screens for patients as they enter the room and begin their surgery, creating a calmer, more relaxing environment.
What does the second phase of the surgical suite upgrade entail?
All of the previously mentioned equipment is wonderful, but unless you have state-of-the-art cameras, processors and light sources that go with them, the new monitors don't matter as much—in other words, the picture on the screen is only as good as the camera/processor sending the image to the screen. The second phase is focused on the cameras and processors, which are slated to arrive in September.
This equipment is very important when performing minimally invasive or laparoscopic procedures. It's the equipment that provides the image for the surgeon to perform surgery. For example, it shows the inside of the abdomen or the inside of a joint. By having the combination of a high-quality camera, processor and screen, a superior image is created for the surgeon.
The new cameras/system are a Stryker 4K fluorescence platform, allowing surgeons to visualize structures in greater detail and with higher precision. There is improved clarity and more accurate color reproduction. We already have this capability with the da Vinci Xi surgical robot, but now all non-robotic laparoscopic surgeries will have this same advanced image quality. This upgrade brings us into an era of the most up-to-date technology for imaging in the medical field.
How are the different surgical teams responding to all of the upgrades thus far?
 The surgical teams and surgeons are very excited about these upgrades. It has been a much needed change, and it brings our surgical suites to the same level as what you would find in a larger tertiary hospital.
The surgical teams and surgeons are very excited about these upgrades. It has been a much needed change, and it brings our surgical suites to the same level as what you would find in a larger tertiary hospital.
In fact, this can help with recruiting future surgeons—having cutting-edge operating rooms is attractive to new surgeons who may prefer to work in a rural or community hospital, but don't want to sacrifice having lower quality or older technology. New surgeons are often trained in hospitals with advanced technology, and having this upgrade can increase their interest when considering Door County Medical Center.
And what has been the takeaway regarding the upgrades?
From the broadest perspective, all of us have felt that the biggest upgrade has been integration—the complete integration of technology in the surgical suites. For example, if a surgeon is at the operating table and wants to look at an x-ray or CT scan, with the new equipment and integration, the nurse can pull that image up at the central hub, send the image to a screen, and the surgeon doesn't have to move. Instead, they can remain at the bedside, and the screen can pull right up to the surgeon for viewing. In the past, we would pull the image up on a small desktop computer screen and the surgeon would walk over to it for viewing.
There is so much more at our fingertips now. The anesthesiologist can transmit all of the vital signs—the blood pressure, the pulse, the EKG rhythm—to a screen, making it easier for the entire team to see and be aware of this data during the surgical procedure.
From the outside, all of these changes and upgrades may not seem like much, but having full integration and improved image quality with this surgical suite technology is a game changer.
What is the effect of all of these upgrades to the patients undergoing procedures at DCMC?
 It makes all aspects of the surgery faster—everything is more efficient. Decreasing the time a patient spends in the operating room reduces risk to patients. Less time spent doing a procedure and being under anesthesia can reduce the patient's recovery time. Having clear and high quality images, allows greater ease for the surgeon to perform the surgery. All of this allows patients to recover more quickly, improving their outcome. Also, every minute in the operating room is expensive and having these improved efficiencies, reduces cost.
It makes all aspects of the surgery faster—everything is more efficient. Decreasing the time a patient spends in the operating room reduces risk to patients. Less time spent doing a procedure and being under anesthesia can reduce the patient's recovery time. Having clear and high quality images, allows greater ease for the surgeon to perform the surgery. All of this allows patients to recover more quickly, improving their outcome. Also, every minute in the operating room is expensive and having these improved efficiencies, reduces cost.
Our overarching goal is to facilitate high quality equipment for our surgeons, thereby creating a safe environment for the patient—one that follows best practices. At the end of the day, patient safety and their experience is the reason for any upgrades. Surgery can be scary. If we can make operating room time more efficient, while maintaining safety, thereby reducing our patient's recovery times and improving outcomes…,then all of these updates are worthwhile.